The College of Urgent Care Medicine
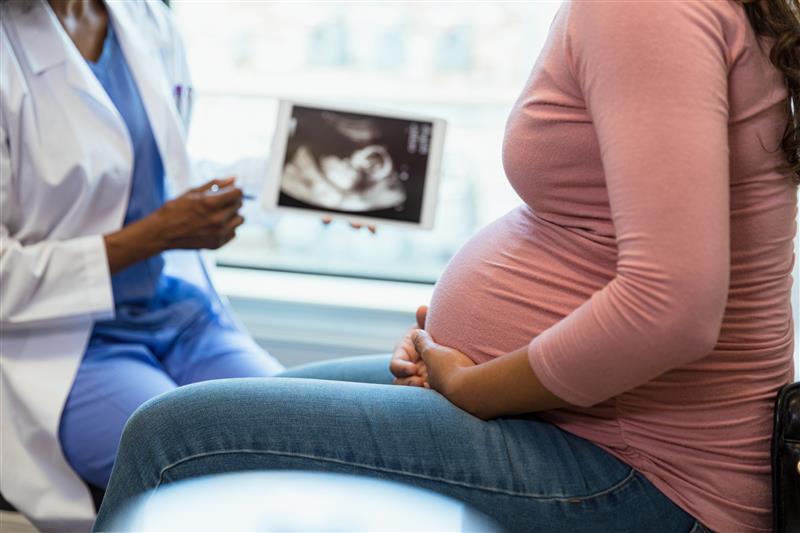

Maternal health is important across all healthcare settings. Find free protocol resources from the American College of Obstetricians and Gynecologists to help inform your practice, below.
ASK ABOUT PREGNANCY
HAVING A PLAN AND KNOWING REFERRAL OPTIONS AHEAD OF TIME CAN BE LIFE-SAVING