Brian Sun, DMD, MS
Oral & Maxillofacial Surgeon (“OMFS”)
The prevalence of dental implants has reached a record high in recent decades. Approximately 6% of the U.S. population had at least one endosseous oral implant by 2015, which represents an 8-fold increase from 1999 that continues to rise.[1] Some projections estimate that up to a quarter of American adults will undergo implant placement in the next decade. Consequently, non-dental healthcare providers are increasingly encountering inflammatory emergencies arising from dental implant failure.
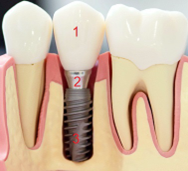
A typical dental implant complex consists of the crown, the abutment, as well as the implant screw (Figure 1). The crown is the white, esthetic portion that replicates the visible portion of a native tooth (#1). The implant is the titanium- or zirconia-based screw that is inserted into the underlying jawbone (#3). The abutment serves as the interphase between the two (#2). Although any components could contribute to failure, most complications occur at the level of the implant screw itself because it directly integrates with the living tissues.
A healthy implant forms a watertight attachment to both the surrounding mucosa (also known as the gingiva) and the underlying bone. If bacterial biofilms of Fusobacteria, Prevotella, and/or Streptococci species form at this interface, the mucosa may inflame and partially detach from the implant, creating a sulcus.[2] An inflamed mucosa would demonstrate erythema, tenderness, hyperplasia, swelling, and potentially bleeding adjacent to the dental implant.[3]
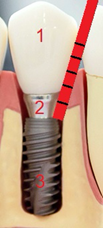
The healthcare provider must first distinguish the extent of the inflammatory disease using a periodontal probe. A periodontal probe is a thin, probe-like ruler (Figure 2). Its tip should be introduced gently through the sulcus to measure the distance from the mucosal surface to the attachment point between the implant and bone (Figure 3). Probing depths of 3mm or less is indicative of peri-implant mucositis (PIM) where the mucosa is inflamed but the underlying bone remains relatively unchanged. [4] Depths 4mm or greater indicates peri-implantitis (PI) where the underlying bone has been destroyed. (Figure 4). Nonmetallic probes are preferred and available at most reputable medical-dental suppliers such as Henry Schein® and Patterson®.

Nonmetallic construction is critical as metallic instruments can abrade or damage implant surfaces, creating additional biofilm attachment sites.[5] For both PIM and PI, the provider should use a fine, non-metallic instrument to debride the sulcus. The periodontal probe itself can be used to remove any visible residue. Thicker angiocaths 18g or wider may also be used as they offer flexible tips and can be used to directly irrigate into the debrided areas. Other common and affordable instruments include commercial dental picks such as the Sunstar GUM Soft-Pick® which are equipped with textured surfaces for debris trapping. Irrigation can be conducted using saline or, more preferably, using a topical antibiotic solution such as 0.12% chlorhexidine gluconate. Clinicians may prescribe additional chlorhexidine for at-home use as a mouth rinse until the patient can visit their dental professional.
Peri-implantitis (PI) represents a worsening progression of peri-implant disease but with comparable bacterial populations. Its histology shows increased presences of neutrophils, B-cells, and macrophages when compared to PIM, leading to active destruction of bone.[6] Later stages of PI may be accompanied by frank purulence and implant mobility as well.[7] Treatment should consist of the same debridement process, though a 3% hydrogen peroxide is likely a more effective irrigant. Long-lasting topical antibiotics may be helpful in arresting progression of the bone loss.[8] Minocycline microspheres are commercially available (Arestin™) and sold in injectable syringes. Chlorhexidine is also manufactured in small chips (PerioChip™) and can be placed in any debrided spaces. Although not ideal, clindamycin powder (found within PO clindamycin capsules) can also be placed within the sulcus using small nasal or otic/ear scoops.
Fortunately, outright peri-implant abscesses are quite rare. This is likely because the microbial colonization occurs at or near the surface of the mucosa, which allows for ready drainage of any purulence. If present, they should be treated like any intraoral abscesses and drained via incision and/or aspiration.
Systemic antibiotics can be used especially in the later stages when purulence becomes evident. Beta-lactams such as amoxicillin, penicillin, and cephalexin – a mainstay for traditional odontogenic infections – should be augmented with clavulanate (in the form of combined amoxicillin-clavulanate 875-125mg formulations) or with metronidazole (usually dosed at 500mg three times daily) to help better address the anaerobes present in PI.[9] Other suitable antibiotics may include azithromycin (500mg qday 1st day, 250mg qday 4 following days) or doxycycline (100mg twice daily) as outlined by the American Heart Association infective endocarditis guidelines.[10] All PI patients must be reminded of good oral hygiene and instructed to visit his or her dental care provider as soon as possible.
It is important to note that systemic metabolic imbalances frequently fuel rapid progression to PI and irreversible bone loss despite adequate treatment of PIM. In particular, poorly managed diabetes mellitus (both type 1 and 2) is associated with increasing rates of implant failures [11] as are osteoporosis and metastatic cancer.[12] Long-lasting topical antibiotics and systemic antibiosis should be considered for these patients even if they did not show evidence of PI. As always, excellent patient interview and history taking is critical.
It is important to note that this article is not meant to direct any treatments or diagnoses. The information presented represents our own protocols and is presented for your academic consideration. All clinical decisions should be made based on the knowledge and experience of appropriately licensed providers.
H. Brian Sun, DMD, MS
Oral & Maxillofacial Surgeon (“OMFS”)
Clinical Assistant Professor, Western University of Health Sciences
Clinical Instructor, University of the Pacific
References
[1] Elani HW, Starr JR, Da Silva JD, Gallucci GO. Trends in Dental Implant Use in the U.S., 1999–2016, and Projections to 2026. Journal of Dental Research. 2018;97(13):1424–30.
[2] Pokrowiecki R, Mielczarek A, Zaręba T, Tyski S. Oral microbiome and peri-implant diseases: Where are we now? Therapeutics and Clinical Risk Management. 2017;13:1529–42.
[3] Heitz-Mayfield LJA, Salvi GE. Peri-implant mucositis. Journal of Clinical Periodontology. 2018;45(August 2017):S237–45.
[4] Pontoriero R, Tonelli MP, Carnevale G, Mombelli A, Nyman SR, Lang NP. Experimentally induced peri-implant mucositis. A clinical study in humans. Clinical Oral Implants Research. 1994 Dec 1;5(4):254–9.
[5] Prathapachandran J, Suresh N. Management of peri-implantitis. Dental research journal. 2012 Sep;9(5):516–21.
[6] Schwarz F, Derks J, Monje A, Wang HL. Peri-implantitis. Journal of Clinical Periodontology. 2018;45(June 2016):S246–66.
[7] Stavropoulos A, Bertl K, Pietschmann P, Pandis N, Schiødt M, Klinge B. The effect of antiresorptive drugs on implant therapy: Systematic review and meta-analysis. Clinical oral implants research. 2018 Oct;29 Suppl 1:54–92.
[8] Renvert S, Lessem J, Dahlén G, Lindahl C, Svensson M. Topical minocycline microspheres versus topical chlorhexidine gel as an adjunct to mechanical debridement of incipient peri-implant infections: a randomized clinical trial. Journal of Clinical Periodontology. 2006 May 1;33(5):362–9.
[9] Blanco C, Pico A, Dopico J, Gándara P, Blanco J, Liñares A. Adjunctive benefits of systemic metronidazole on non-surgical treatment of peri-implantitis. A randomized placebo-controlled clinical trial. Journal of Clinical Periodontology. 2022;49(1):15–27.
[10] Wilson WR, Gewitz M, Lockhart PB, Bolger AF, Desimone DC, Kazi DS, et al. Prevention of Viridans Group Streptococcal Infective Endocarditis: A Scientific Statement from the American Heart Association. Circulation. 2021;143(20):E963–78.
[11] Jiang X, Zhu Y, Liu Z, Tian Z, Zhu S. Association between diabetes and dental implant complications: a systematic review and meta-analysis. Acta Odontologica Scandinavica. 2021;79(1):9–18.
[12] Schimmel M, Srinivasan M, McKenna G, Müller F. Effect of advanced age and/or systemic medical conditions on dental implant survival: A systematic review and meta-analysis. Clinical Oral Implants Research. 2018;29(March):311–30.